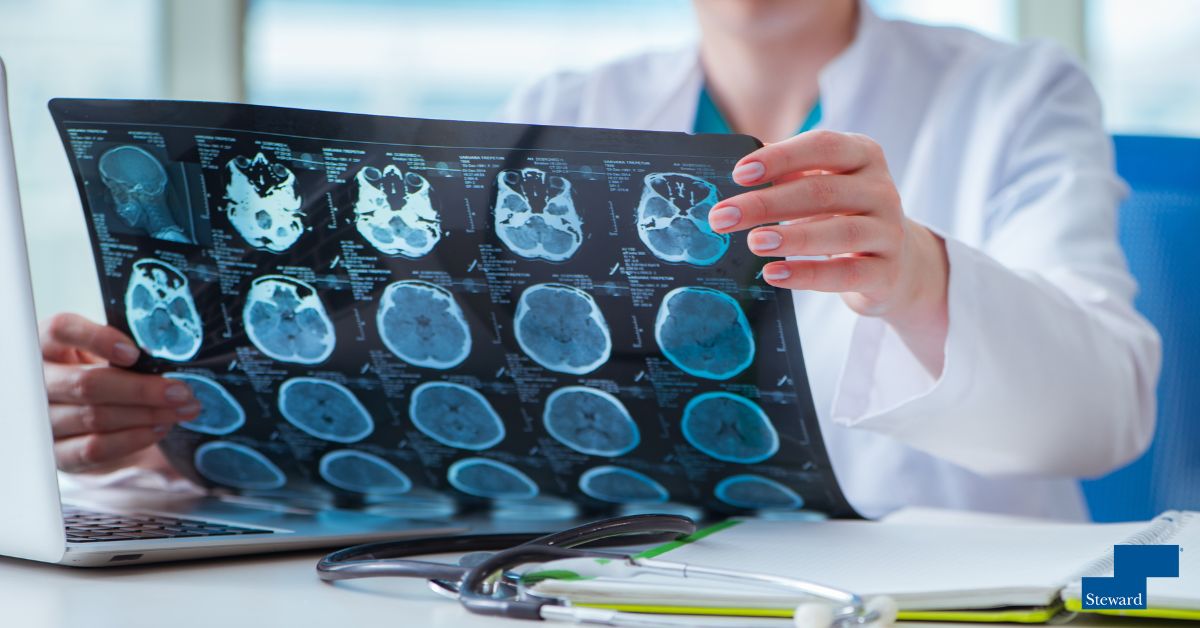
July 19 will mark the 5th Annual Glioblastoma Awareness Day
Glioblastoma (GBM) Awareness Day takes place each year on the third Wednesday of July to recognize the impact of this devastating disease, which is the deadliest type of primary brain cancer. It is intended to highlight the national need to raise awareness, advance research, and further take action to take better care of GBM patients, prolong life, and ultimately cure glioblastoma. The National Brain Tumor Society spearheaded this annual event starting in 2019: Glioblastoma Awareness Day (braintumor.org)
 To highlight this awareness day, Dr. Ekkehard Kasper, Chairman of Neurosurgery and Dr. Fred Lam, attending neurosurgeon at St. Elizabeth’s Medical Center, a Steward family hospital discuss glioblastoma in the following Q and A to help others learn more about this challenging cancer.
To highlight this awareness day, Dr. Ekkehard Kasper, Chairman of Neurosurgery and Dr. Fred Lam, attending neurosurgeon at St. Elizabeth’s Medical Center, a Steward family hospital discuss glioblastoma in the following Q and A to help others learn more about this challenging cancer.
Who does Glioblastoma affect?
Glioblastoma (GBM) is a disease that all Americans should care about. It can strike anyone, including men, women, and children of any age, background, and walk of life. It does not discriminate on race, gender, socioeconomic status, region, or age.
 Why is it important for to raise awareness of this devastating disease?
Why is it important for to raise awareness of this devastating disease?
Glioblastoma (GBM) is one of the most common yet highly complex, treatment-resistant, and therefore fatal cancers. The mean age at diagnosis is 65 and more than 14,490 Americans are expected to receive a new GBM diagnosis in 2023. GBM accounts for about 50% of all primary malignant brain tumors and it is estimated that more than 10,000 individuals in the United States will succumb to glioblastoma every year.
How does GBM affect an individual?
In addition to being life-threatening in itself – and its harsh treatment side effects – GBM profoundly affects the brain function, with an impact on cognition, mood, behavior, and the function of every organ and body part. Many patients will lose their ability to work, drive, and a host of other functions that contribute to one’s sense of self and independence. Glioblastoma is also one of the more expensive cancers to treat, often leaving patients and families with major financial hardship on top of the burdens of the disease.
What are the survival rates of glioblastoma?
The five-year survival rate for glioblastoma patients is only 6.9 percent, and the average length of survival for glioblastoma patients is as low as 8 months. Survival rates and mortality statistics for GBM have remained virtually unchanged for decades.
Is one health care population more prone to develop GBM than others?
Doctors don’t know what causes Glioblastoma. Like other cancers, it starts when cells begin to grow uncontrollably and form tumors. This cell growth may have something to do with gene changes. You’re more likely to get this type of tumor if you’re: Male, age 40 or older, of European or Asian heritage.
Are there many drug options to treat GBM?
Despite being identified in the scientific literature as early as the 1920s as the first malignant brain tumor, there have essentially only been four drugs and one device ever approved by the FDA specifically for the treatment of glioblastoma. None of these treatments have succeeded in significantly extending patient lives beyond a few extra months.
What makes treating glioblastoma so challenging?
Because glioblastoma multiforme rarely spreads, the problem that doctors face with this tumor is how it grows and places pressure on the critical structures of the brain. Unlike other tumors, the GBM grows by infiltrating the brain itself and becoming part of its fabric, with “tentacles” that secure its position. This makes it virtually impossible to remove some GBMs when they form because they are so securely woven into the brain tissues. The same is true for spinal cord GBMs.
Surgery is often recommended to remove as much of the tumor as possible, however, because this will relieve some pressure and prolong life. This is true even with the rare inherited form of this malignant tumor. There is the possibility of putting this tumor into remission in certain instances, but because the cancer is so aggressive, it can usually defeat radiation and chemotherapy over time.
Age, ability to carry on ordinary daily activities and specific treatment management (based on gene profiles in a subset of GBM patients) are the biggest factors to contribute to a favorable outcome in affected patients. Much has been learned recently about the individual DNA fingerprint and overall makeup of these tumors. Many treatment options are at or near a clinical trial stage and there is a lot of hope on the horizon. Glioblastoma multiforme does not have to win its onslaught on patients. There can be more survivors, but we must support more research into this field to make that happen.
What are signs and symptoms individuals can be mindful of to share with their doctor if they are experiencing symptoms?
The typical symptoms of glioblastomas include headaches, nausea and vomiting, sleepiness, confusion, personality or mood changes, double vision or blurred vision, loss of appetite. Also, progressive loss of brain function (such as speech, strength, or memory):
- Weakness on one side of your body
- Memory loss
- Problems with speech and language
- Muscle weakness
Seizures, which may be associated with increased intracranial (within the head) pressure. CT and MRI scans with and without contrast are usually used to identify the tumors before a biopsy will diagnose glioblastoma.
There has been recent news surrounding new medications to treat glioblastomas. Can you comment?
We currently have 4 established drugs— and one device — which have been approved by the FDA specifically for glioblastoma.
- Temozolomide (Temodar)—Chemotherapy drug
FDA approved 2005 for treatment of adult patients with newly diagnosed GBM - Bevacizumab (Avastin)
FDA approved 2009 for treatment of patients with recurrent GBM and prior treatment - Polifeprosan 20 with Carmustine Implant (Gliadel)
FDA approved 1997 for treatment of initial occurrence GBM, an alkylating agent that is surgically implanted as a wafer after surgical resection and allows for drug delivery directly to the tumor site - TTF Device
FDA approved 2011 approved as a medical device for adult patients with recurrent GBM after surgery and chemotherapy treatment to deliver electric tumor-treating fields to the brain to physically break up the tumor cell membranes. - In addition, patients are offered extensive CLINICAL TRIALS:
The NBTS Clinical Trial Finder provides information obtained from ClinicalTrials.gov, a service of the U.S. National Institutes of Health, providing information on publicly and privately supported clinical studies of human participants with locations in all 50 States and in 196 countries.The trials involve many types of therapy, including but not limited to immunotherapy, antiangiogenic therapy, viral therapy, and targeted therapy (personalized medicine).
At St. Elizabeth’s , how are we making a difference for patients who have a glioblastoma, and their families/support system?
As a highly specialist team of providers, we ensure a timely diagnosis and surgical intervention for all patients with a Glioblastoma. All patients are jointly reviewed at our weekly multidisciplinary brain tumor conference. We ensure that all patients are referred to the appropriate center for adjuvant care and they will be seen in a timely manner as time is of the essence in these devastating brain tumors. Our designated brain tumor program coordinator, Maddy Curry, RN, will make sure that no one is lost in the labyrinth of institutions and care providers.
We also ensure that all patients have access to all available resources including ABTA resources, NBTS resources, physical, occupation and speech therapy, support groups, etc. and that we are always available as a resource for all our patients. We emphasize that we always care for the whole patient, including their loved ones and their caregivers. We are committed to continuing to do the necessary research to learn more about GBM to make sure that our up-to-date knowledge allows us to provide best care, now and in the future.
Dr. Kasper will be a featured speaker during Glioblastoma International Awareness Day. See more at: https://www.tumorsection.org/
To find a doctor or schedule an appointment, visit Steward DoctorFinder™.